I thought I had breastfeeding figured out. I had breastfed two babies, counseled and consoled countless new moms, and worked through trials and pain myself.
And then I had my third baby.
About this time last year, Angela of Basking Babies was preparing her first Oral Anatomy Conference for Des Moines. I was honored that she had asked me to speak about the chiropractic and cranial role in pre- and post- tongue and lip tie releases. I had recently been seeing more infants in my clinic for care specific to this and was excited to share my experience as a practitioner and spread the word about the importance of chiropractic care and craniosacral work in this population. My only hesitation was that I was due to have our third baby within the month before the conference.
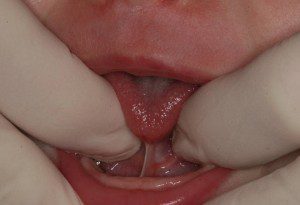
Fast-forward five months. Our daughter had just been born, and the moment after I adored her sweet cheeks and beautiful blue eyes, as she stuck her tongue out over and over again, I looked at my midwife and said, “Thank God, she doesn’t have a tongue tie!” She was sticking her tongue out so far and latched on easily for her first feeding.
Throughout that first day, she ate well, slept often, and pooped that tarry meconium a couple times. Life as a family of five seemed to be on a peaceful track.
When we followed up with our nurse the next afternoon, I explained to her that I felt like things were going pretty well, except for the fact that my nipples were very sore already. She recommended I have the midwives call in a prescription of Jack Newman’s Nipple Ointment (a compounded cream to help keep the area from getting infected. LADIES… this stuff is magical if you have any nipple trauma from nursing!). When she weighed our daughter, her weight was down, but this wasn’t uncommon. She said she would have the lactation consultant check in with me and told me to just keep feeding baby as we had been.
Soon, my baby’s stools were less frequent and her latch was still very uncomfortable, especially on the left side. By day four, Char Wade, the first lactation consultant we saw, suggested I start to offer the breast, then pump and syringe feed my baby every couple hours. The reasons were simple: make sure baby was getting enough calories and make sure I continued to establish an adequate milk supply. This seemed so daunting. Every two hours, day and night, I continued this regime—nurse, pump, feed; then label and store milk, and wash my pump parts for the next feeding.
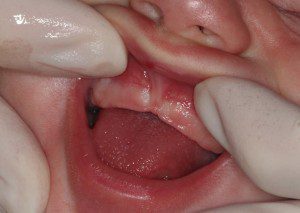
As the sun began to set, my heart began to sink—another long night of little sleep and frequent feeds was ahead. Char brought LeeAnn Albright, IBCLC, on board, and the two of them together were my saving grace in this journey. I kept up with regular weighted feedings to see how much milk our baby was transferring, and they watched me nurse and analyzed her latch. Ultimately, they came to the opinion that my baby had a possible upper lip and posterior tongue tie. Although she could stick her tongue out far, she couldn’t lift it up high enough in her palate to effectively transfer milk from my breast, and the restriction in her upper lip was limiting her ability to create a good latch with adequate suction.
Their recommendation was to see Dr. Jenifer Wolfe, a pediatric dentist in Altoona, for a consult. After doing some of my own research and talking with patients and acquaintances about their experiences, I felt the most comfortable with seeking out a pediatric dentist, as opposed to an EENT, whose standard of care seemed to be using scissors as well as often recommending anesthesia because of the large amount of blood. It was important to me that if we needed a release done, that a cold laser would be used (less blood, less chance of infection, quicker, and most importantly, no anesthesia needed).
I was desperate for any advice about anything that could help, and I felt like I couldn’t get into the dentist’s office soon enough. We also called Dr. Mindy Hochgesang, DMD, in Clinton, Iowa, who is well known across the state for her work with tongue and lip releases, but we were able to get into Dr. Jen sooner.
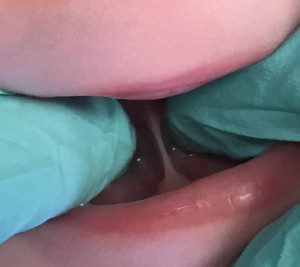
On a Monday morning, when my daughter was 11 days old, we took her to her first appointment with a dentist, in hopes of a miracle of sorts. My stomach churned and my anxiety took over as my husband drove us there. I knew that if the doctor found that there was not only extra tissue, but also that the function of her suck was altered, she would recommend the tissue be released.
Her office was amazing and made us feel very welcomed. They took us back into our room, and the assistant took our history, explained what Dr. Jen would be looking at, and answered basic questions we had. Then the doctor came in and examined our daughter as she lay on her back on my lap. She explained what she was seeing—that there was an extended frenulum under the tongue and at the upper lip. Her tongue would lift up on the sides with sucking, but not in the center, and those areas of restriction felt tight and wouldn’t stay red with pressure.
Her recommendation? That we have the procedure done to release these restrictions.
She would wrap our daughter in a swaddle blanket, place protective googles on her eyes, and then use a laser to quickly release the tissues while her two assistants helped hold our daughter’s mouth open. Dr. Jen assured us the procedure would be quick and minimally painful.
I broke down in tears. I had done everything in my power throughout my pregnancy, delivery, and her first days of life to keep things peaceful and low intervention in her life, and now I was about to agree to this. But, I knew this would most likely change our breastfeeding relationship, which would provide so much more benefit than leaving the ties be.
I walked out of the room to set up our follow-up appointment, and before I was done, we got the call to come back into the room. My baby was there, smiling up at me, and I quickly brought her to the breast. She latched on, and it was painless. I cried with relief, but also from some remaining guilt if what I had just done was the right choice.
After the Procedure
We were assured things went well and instructed on home care. Exercises were demonstrated that would help decrease the likelihood of reattachment, and pain options were discussed. In preparation for the procedure, we had given her Rescue Remedy homeopathic drops and arnica pellets in her mouth that dissolved quickly as I held them against her cheek right before the release. I gave these to her every 15 minutes after the procedure for the first hour, every hour for the next five, and then as needed after that.
In an attempt to do the stretches often enough, I tried to use diaper changes as my reminder to place her on my legs, face up with her head at my knees, and use my two pointer fingers to lift the upper lip and then my thumb for cross-friction, and then my thumb to lift and tip back the tongue and then cross-friction. I tried to avoid doing this right before feedings, as I didn’t want to create any aversions to feedings. I also adjusted her and did cranial work two to three times per week for a couple weeks.
From that day forward, our baby girl gained weight at a rapid pace, and by the sixth week she was transferring the amount of milk she needed from the breast on her own without the need for supplementations. At six months, she has doubled her birth weight and breastfeeding is a breeze. My supply is ample enough to donate extra milk to other moms in need. In a heartbeat, I would endure the sleepless night, painful feedings, and hard choice to have the release done in order to have the breastfeeding relationship we have now.
What I want you to know…
- Breastfeeding isn’t always easy, even for a veteran.
- Just because your baby looks like his or her tongue or lip may be tied, unless function is altered, no action may be required.
- On the flip side, even if latch seems perfect and is painless, but baby is not gaining weight adequately, is colicky, gassy, fussy at the breast and arching his or her back, falling asleep at the breast without finishing a feeding, or chewing on the nipple, your baby may need to be evaluated by an experienced lactation consultant. Although nursing may not seem to be affected, speech, digestion, and dental health may be!
- Early detection is CRITICAL. I suggest every new mom seek out the help of an experienced lactation consultant, even before your baby is born. And then keep her number on speed dial! Locally, check out:
- Angela Sweiter, IBCLC, of Basking Babies (home visits and monthly classes for new and expecting moms)
- LeeAnn Albright, IBCLC, of Nature’s Best Lactation (home visits and monthly breastfeeding support groups, as well as classes)
- Willowsong Midwifery Clinic’s MotherBaby Café (hours open to the public and at no charge) with Char Wade and LeeAnn Albright
- Your pediatrician or EENT may not be as experienced with tongue and lip ties and may minimize the need for this procedure. Please, start with an experienced lactation consultant.
















This was such a good read. I wish I had been more informed about this issue. I had such difficulty with my daughter but kept going through it all. That is until she was popping off so frequently at 5 months that I was beyond frustrated. Went to a dentist, even though my regular doctor said she looked fine, and she had a class 5 lip tie and a little tongue tied. We decided to clip her lip and that next feeding was like she was a new child. We then went to Angela and she examined her and let me know she had a high palate as well and helped me tweak positioning to help her nurse. And we’ll, here we are at almost 16 months! Thank you all for everything you do!
so the pain with latching went away immediately after having the ties released? I had my three week old son’s upper lip tie released last week but am still in pain. He also has a posterior tongue tie and will most likely get it released on Tuesday. I just don’t know how much longer I can take the pain. Many people say it’s worse before it’s better…what was your experience?
My son is now 4 months old and had both lip and tongue tie. We had laser procedure done at 2 months and it took a good month for breastfeeding not to hurt. We had to see a cranial therapist a couple of times after as well. Do not give up I kept hearing from people that it was going to be pain free right after but that wasn’t the case for us. Again it took him about a month to learn how to get the sucking motion right and have a good latch after the procedure.
Both my babies were tongue tied. Baby #1 had a posterior tongue that didn’t get clipped until 6 weeks, so although I noticed an improvement in latch pretty soon, my nipples were extremely traumatized and took another couple of weeks to heal. I hope it gets better for you soon! I can SO relate to feeling like you just can’t take it anymore. But in the end, I am glad I stuck it out because I finally got to the point where I enjoyed breastfeeding and that was a wonderful bonding experience.
Thank you for sharing this info! My daughter (now age 3) was tongue-tied at birth and we had it clipped when she was 6 days old. We were referred to an ENT but I had no idea that a dentist could also help. We did not have success at breastfeeding so I definitely want to pay more attention to this when my baby boy is born in June!